Intergenerational Transmission of Mental ill health
This policy briefing paper was written by Dr Simona Rasciute from Loughborough Business School based on the analysis done in collaboration with Louise Vesely-Shore MBE, Ella Marley-Zagar and Alena Nash of the Office for National Statistics (ONS).
Read the Full Report on the ONS website.
Why parental mental health must be a central consideration to child mental health policy
Mental health disorders now account for a substantial share of the disease burden among young people in England. Rates of stress, anxiety and depression continue to rise, placing pressure on schools, NHS services and local authorities.
Policy responses have largely focused on schools and child-centred interventions. However, children’s mental health does not develop in isolation. It is shaped by family environments, parental wellbeing and wider socio-economic conditions.
Evidence suggests mental health problems are correlated across generations, but until now research has relied on small samples, self-reported measures, or focused primarily on mothers. There has been limited large-scale for England that includes both parents.
Research carried out by Dr Simona Rasciute, Loughborough University, in collaboration with the Office for National Statistics, seeks to understand this relationship better.
Research
The study develops a novel population-wide data infrastructure for England linking:
- Children’s NHS hospital and emergency care records (Hospital Episode Statistics and Emergency Care Dataset)
- Children’s educational records (National Pupil Database)
- Mothers’ and fathers’ NHS hospital, emergency care and Talking Therapies records
- Census 2021 socio-economic and household characteristics
- Neighbourhood deprivation and green space data from Ordnance Survey.
This is the first large-scale administrative data linkage in England connecting both mothers’ and fathers’ health and socio-economic records to children’s health and education outcomes.
Sample
The study primarily analyses data on approximately 1.1 million children who were aged 5 to 16 and living in two parent households Census (21 March 2021), who undertook primary (key stage 1 or 2) or secondary (key stage 4/GCSE) assessments in summer 2022 (academic year 2021/22). Health data for adults and children captures contact with health services for specificconditions between April 2021 and March 2022.
Results
Using advanced matching methods to estimate causal effects, the study finds:
Strong intergenerational transmission
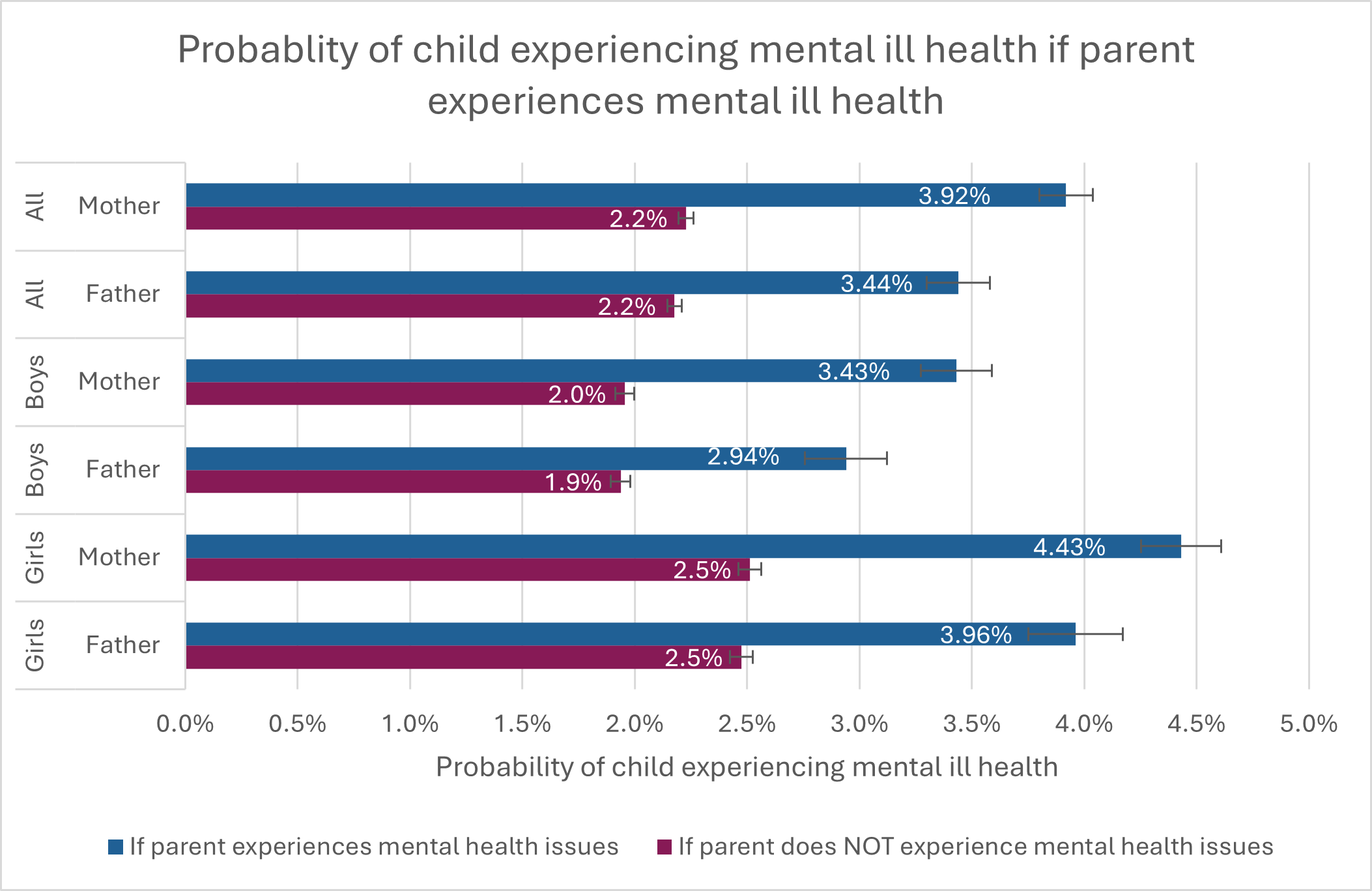
- Around 2–5% of children experience clinically recorded mental health problems.
- This nearly doubles when the mother has mental health issues.
- It increases by around 50–60% when the father has mental health issues.
- Effects remain statistically significant across alternative model specifications, household types and longer time horizons.
Fathers matter: paternal mental ill health has a sizeable and independent causal effect on child mental health. For boys, when both parents experience mental ill health, the probability of experiencing mental ill health is amplified.
Risk is gendered: effects are present for both boys and girls but are larger for girls.
A child’s mental health is shaped by multiple factors
Children are more likely to experience mental health problems if they
- have chronic physical health conditions
- are young carers
- have
- have lower attainment in maths
- live in less green or more deprived neighbourhoods
Impact of child mental ill health
As well as exploring the drivers impacting child mental health, the study finds:
The relationship is bi-directional, with children’s mental health affecting their parents’ mental health:
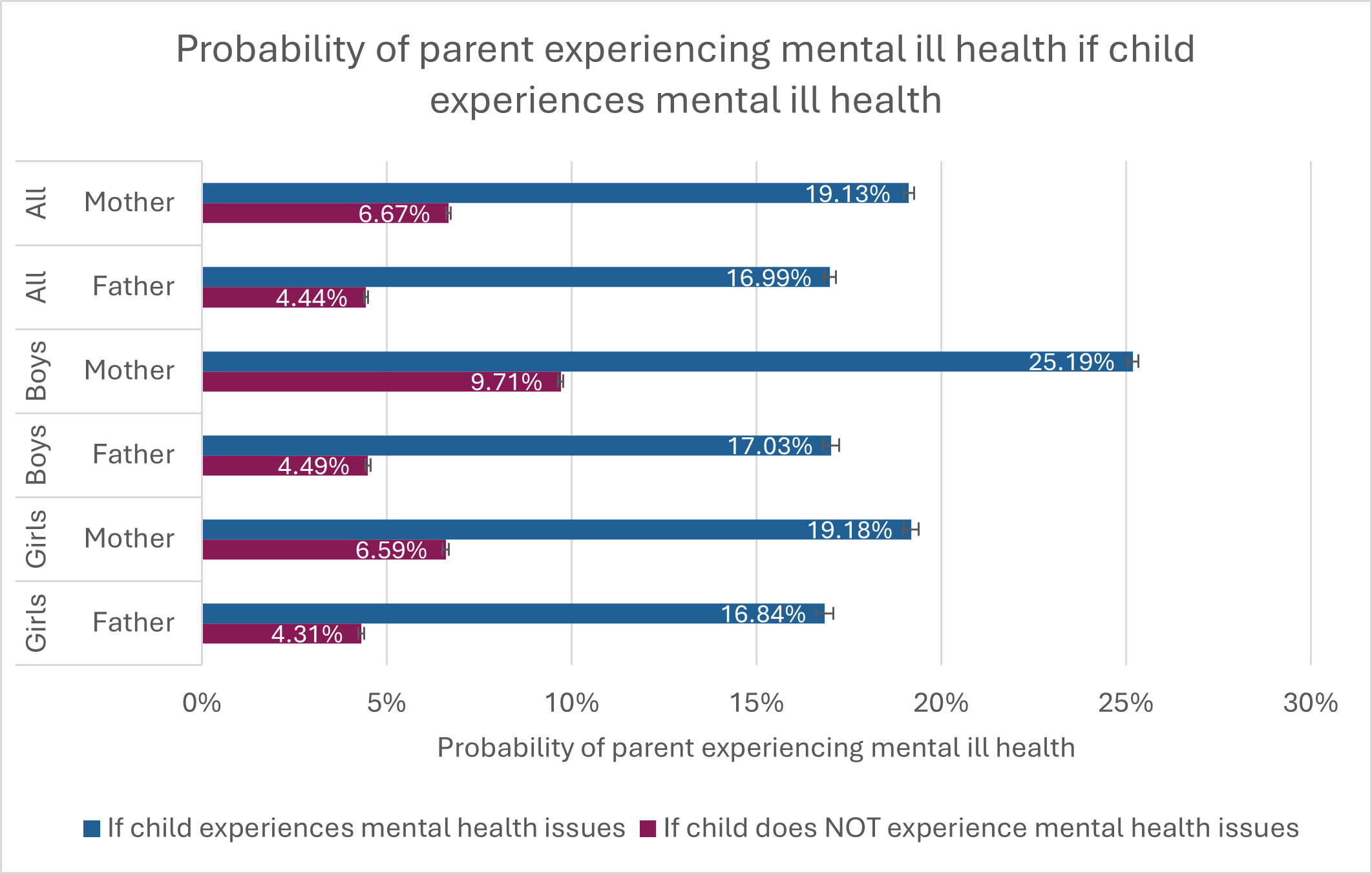
- findings show that when children experience clinically recorded mental health problems, parents/carers are around three times more likely to experience mental health problems.
- This effect is greater for mothers with sons who experience mental health problems
Children’s mental health affects their educational outcomes:
- Experiencing mental ill health reduces maths attainment, both directly and via increasing children’s absence from school, which in turn negatively impacts a child’s scores in maths.
Policy recommendations
- Move from child-centred to family-centred mental health policy
Child mental health strategies should systematically incorporate parental mental health. Treating the child alone risks addressing symptoms rather than drivers. This includes:
- Screening for parental mental health difficulties within child services
- Integrated adult–child mental health pathways
- Family-based therapeutic interventions
- Recognise paternal mental health as a policy priority
Paternal mental health has a significant effect but remains under-recognised. Ignoring fathers may limit the effectiveness of interventions. Policy frameworks should:
- Include fathers in perinatal and early years services
- Ensure fathers are engaged in school-based mental health referrals
- Improve uptake of NHS Talking Therapies among men
- Target compounded household risk
Where both parents experience mental ill health, the risk a child will experience mental health issues increases. Local authorities and NHS services should prioritise a family-based ‘whole household’ approach.
- Strengthen cross-sector data integration
The study demonstrates the value of linking health, education and census data. Government should:
- Sustain secure administrative data linkage infrastructure
- Use integrated data for early risk identification
- Embed evaluation within service delivery
- Address wider determinants alongside family factors
Mental health policy should be embedded within broader social policy. This includes:
- Reducing school absence
- Strengthening SEND support
- Investing in neighbourhood environments, including green space
- Tackling area-level deprivation
- Family-based interventions and place-based strategies must work together.
Child mental health problems are not isolated events. They are embedded within family systems and shaped by parental wellbeing and socio-economic context. This study provides robust causal evidence that parental mental ill health - maternal and paternal - significantly increases the risk of child mental ill health in England. Further work to explore the complex interplay of factors which influence child mental ill health would be beneficial, and we are working with ONS to secure agreement to make the linked data asset available to external researchers through the Secure Research Service.