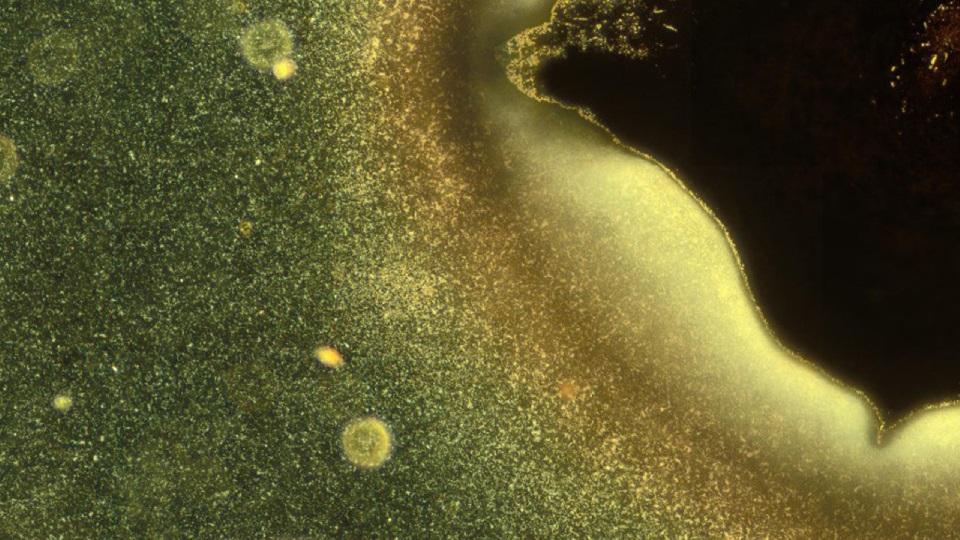
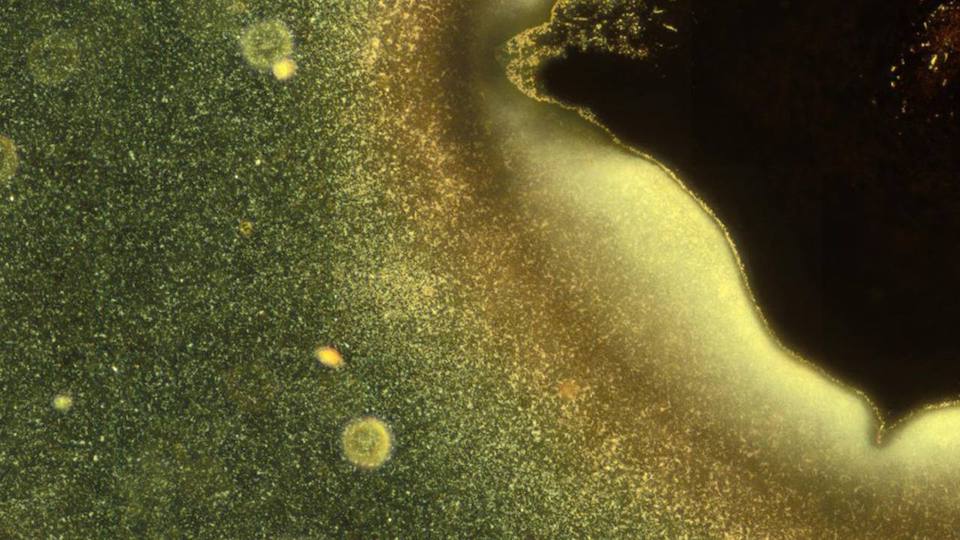
The researchers are currently exploring different bacterial species and their specific strategies of motion and surface colonisation.
The team’s research has the potential to aid in the development of medical applications to treat bacterial infections.
Of the research’s importance, Dr Mazza said: “Microbial life is fundamental for the ecosystem – more complex life forms in soil and water depend on the activity of microbes – and for the human body – our guts contain enormous numbers of microorganisms necessary to protect us and even to produce vitamins.
“Understanding how pathogens operate can provide additional weapons to fight them.”
- Tackling tuberculosis: exploring if chemicals found in corals can prevent the formation of drug-resistant cells and biofilms that make the disease hard to treat
Biofilms are an integral part of organic chemistry expert Professor Andrei Malkov’s research programme focused on tuberculosis (TB) infections.
TB is a global health problem and, according to the World Health Organisation, it took the lives of 1.4 million people in 2019, and a further estimated 10 million people fell ill with the infectious disease last year, which mainly affects the lungs.
There are different forms of TB, some of which are treatable and curable.
However, ‘multidrug-resistant tuberculosis’ (MDR-TB) is a form of TB caused by bacteria that does not respond to the most effective first-line anti-TB drugs, and in severe cases, it also does not respond to the most effective second-line drugs, meaning it remains a public health crisis and a health security threat.
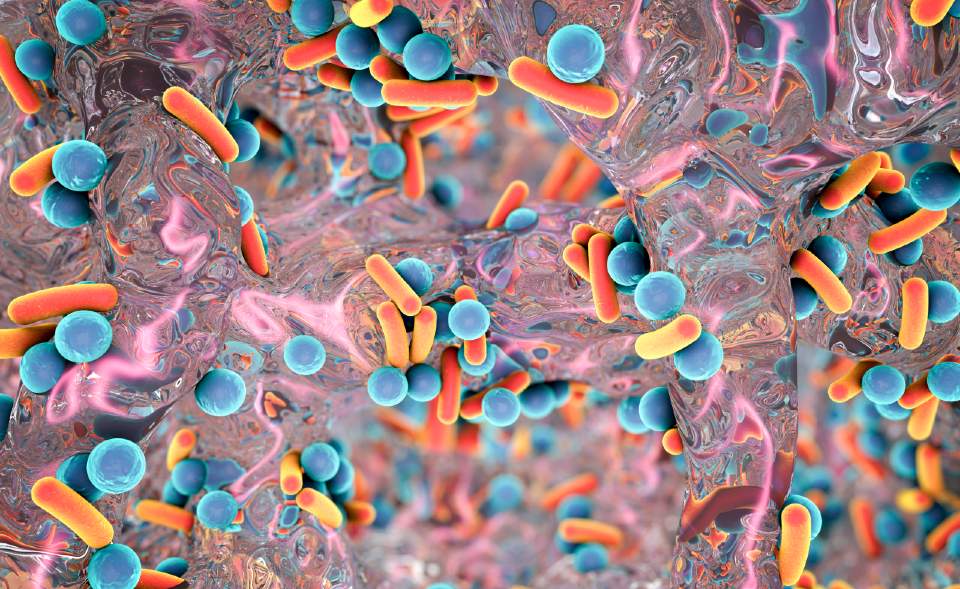
Mycobacterium tuberculosis (M. tb) – the pathogenic bacteria that causes TB – can develop this resistance to antibiotic therapy by producing drug-tolerant cells known as ‘persister cells’.
M. tb also has the ability to form biofilms inside the lungs, as well as on the surfaces of medical devices, that are abundant with these persister cells.
Bacterial persistence coupled with biofilm formation is directly associated with the failure of antibiotic treatment of TB, therefore it is important to continue to search for new drugs targeting the formation of persister cells.
Professor Malkov is working with biologists and chemists to find new, small molecules capable of inhibiting persister cell and biofilm formation in the hope it will lead to more effective antitubercular therapies.
He told VOLUME one of the team’s recent successes is the identification and synthesis of chemical compounds found in a species of soft coral that, during ‘in vitro’ experiments (commonly referred to as ‘test-tube experiments’), exhibited the ability to inhibit persister cell formation and eradicate biofilms formed by M. tb pathogens.
The team, led by the Russian Academy of Sciences, has submitted a paper on the topic and their findings to the journal Cell Chemical Biology and are currently revising the manuscript according to reviewers’ comments.
Professor Malkov commented: “We have identified a small molecule that inhibited formation of biofilms in the laboratory settings.
“The investigation is now focusing on establishing the exact mechanism of action of the new compounds and making further modifications to the compound structure to improve its activity.”
He continued: “The identified bioactive natural product analogue may serve as a promising new lead compound for developing novel antitubercular therapies relying on the suppression of persister cell formation and thus effective against chronic and recalcitrant tuberculosis infections.”
- Developing a rapid, easy, and affordable point-of-care test to detect wound infection
Chronic or non-healing wounds, such as in people suffering from diabetes or burns, is a severe healthcare problem.
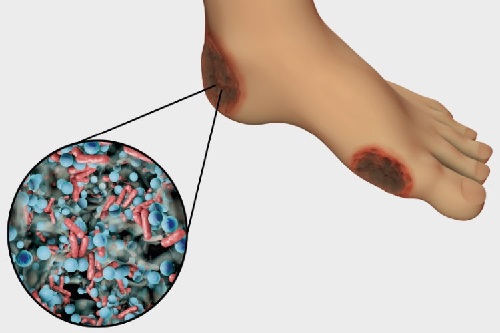
For diabetes alone, among the 55 million people in Europe diagnosed with the condition, the lifetime risk of developing a chronic wound, referred to as ‘diabetic foot ulcer’ (DFU), is as high as 25%. In the UK, the NHS costs due to DFU are £10 billion per year and growing.
Interpreting whether a wound is going to heal or lead to a diseased state is a complex problem and as a result, it is hard to determine the best course of treatment.
Biofilms are the fundamental reason that chronic wounds do not heal in a timely manner and they form when microorganisms – most commonly bacteria - adhere themselves to the wound surface.
However, bacteria can colonize on wounds without causing an infection, so developing a test to simply get a ‘yes/no’ answer for the presence of bacteria is not massively beneficial.
Dr Sourav Ghosh, a healthcare engineering expert, and Praveen Kumar Kaveri, a PhD student in his team of researchers, are developing a rapid, simple, single-step fluorescence-based test that aims to provide crucial information on wound pathogenesis, i.e. whether a wound will heal easily or become non-healing.
The test aims to detect wound infection by determining the number and type of bacteria in a biofilm – known as the ‘bacterial load’ – and then determine the virulence of the bacteria [its ability to prevent wound healing and cause damage to the host].